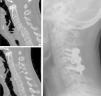
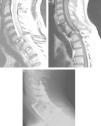
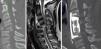
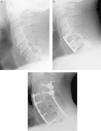
The management of lower cervical spine injuries with a dislocation of one or both facet joints and a displacement of a vertebra over the adjacent stills generates considerable controversy. We describe our experience in surgical approach of these injuries.
MethodsWe present 21 cases treated between 2003-2010. Neurological status was evaluated with Frankel scale. Diagnosis was done by radiograph (XR), computed tomography (CT) and/or magnetic resonance image (MRI). Cervical traction was placed in 10 cases before surgery. Posterior and/or anterior approach was used for reduction and stabilization.
ResultsThe 21 cases presented were treated by surgery. Posterior approach was initially used in 17 cases and complete reduction was achieved in 13 of them. The 4 cases where we only got a partial reduction, surgery had to be delayed for different reasons. Anterior approach was initially used in 4 of the 21 cases. In 3 of them, reduction was previously obtained by traction and the fourth case anterior approach was used initially due to an important spinal cord compression. Permanent stabilization was achieved in 19 of the 21 cases. In 1 of the other 2 cases an important deformity was detected after the anterior approach. The other case had a minimal progression after a posterior approach with no increase in successive check-ups. In the first 10 cases, we used traction before surgery but reduction was achieved only in 3 of them. As the number of cases increased we rather used posterior approach in the first place, without even trying a preoperative traction. There was no case of neurological deterioration after surgery.
ConclusionTranslation/rotation injuries of the lower cervical spine are unstable and surgical treatment must be indicated. It is our impression that posterior approach allows a better reduction and stabilization of this injuries and should be used initially without even trying a preoperative traction.
El tratamiento de las lesiones del raquis cervical inferior con luxación de una o ambas facetas articulares y desplazamiento de una vértebra sobre la adyacente todavía genera una controversia considerable. Describimos nuestra experiencia en el tratamiento quirúrgico de este tipo de lesiones.
MétodosPresentamos 21 casos tratados entre 2003-2010. La situación neurológica fue valorada con la escala de Frankel. El diagnóstico se hizo mediante radiografía (XR), tomografía computerizada (CT) y/o resonancia magnética (MRI). La tracción cervical fue utilizada en 10 casos antes de la cirugía. En su estabilización se utilizó un abordaje posterior y/o anterior.
ResultadosLos 21 casos presentados fueron tratados mediante cirugía. Se realizó inicialmente un abordaje posterior en 17 casos y se consiguió la reducción completa en 13 de ellos. Los 4 casos donde obtuvimos solo una reducción parcial, la cirugía tuvo que retrasarse por diferentes motivos. El abordaje anterior se utilizó inicialmente en 4 de los 21 casos. En 3 de ellos, la reducción se consiguió previamente mediante tracción y en el cuarto caso se utilizó al abordaje anterior inicialmente por la importante compresión medular. Se logró una estabilización permanente en 19 de los 21 casos. En uno de los dos casos restantes, se detectó una importante deformidad después del abordaje anterior. El otro caso presentó una mínima progresión después del abordaje posterior que no se incrementó en los controles sucesivos. En los 10 primeros casos, utilizamos la tracción antes de la cirugía, aunque la reducción se logró unicamente en 3 de ellos. A medida que se incrementaba el número de casos, preferimos emplear el abordaje posterior en primer lugar, incluso sin utilizar la tracción preoperatoria. No se produjo ningún caso de deterioro neurológico tras la cirugía.
ConclusiónLas lesiones por traslación/rotación del raquis cervical inferior son inestables y se debe indicar su tratamiento quirúrgico. Nuestra impresión es que el abordaje posterior permite una mejor reducción y estabilización de estas lesiones y se debería utilizar inicialmente incluso sin intentar una tracción preoperatoria.
Artículo

Si es la primera vez que accede a la web puede obtener sus claves de acceso poniéndose en contacto con Elsevier España en suscripciones@elsevier.com o a través de su teléfono de Atención al Cliente 902 88 87 40 si llama desde territorio español o del +34 932 418 800 (de 9 a 18h., GMT + 1) si lo hace desde el extranjero.
Si ya tiene sus datos de acceso, clique aquí.
Si olvidó su clave de acceso puede recuperarla clicando aquí y seleccionando la opción "He olvidado mi contraseña".