The endoscopic techniques used in pituitary surgery have evolved greatly in recent years. Our objective in this study was to conduct a review of the systematic reviews published in the English language literature, to examine their consistency and conclusions reached following studies comparing microsurgery and endoscopic surgery in hypophyseal surgery.
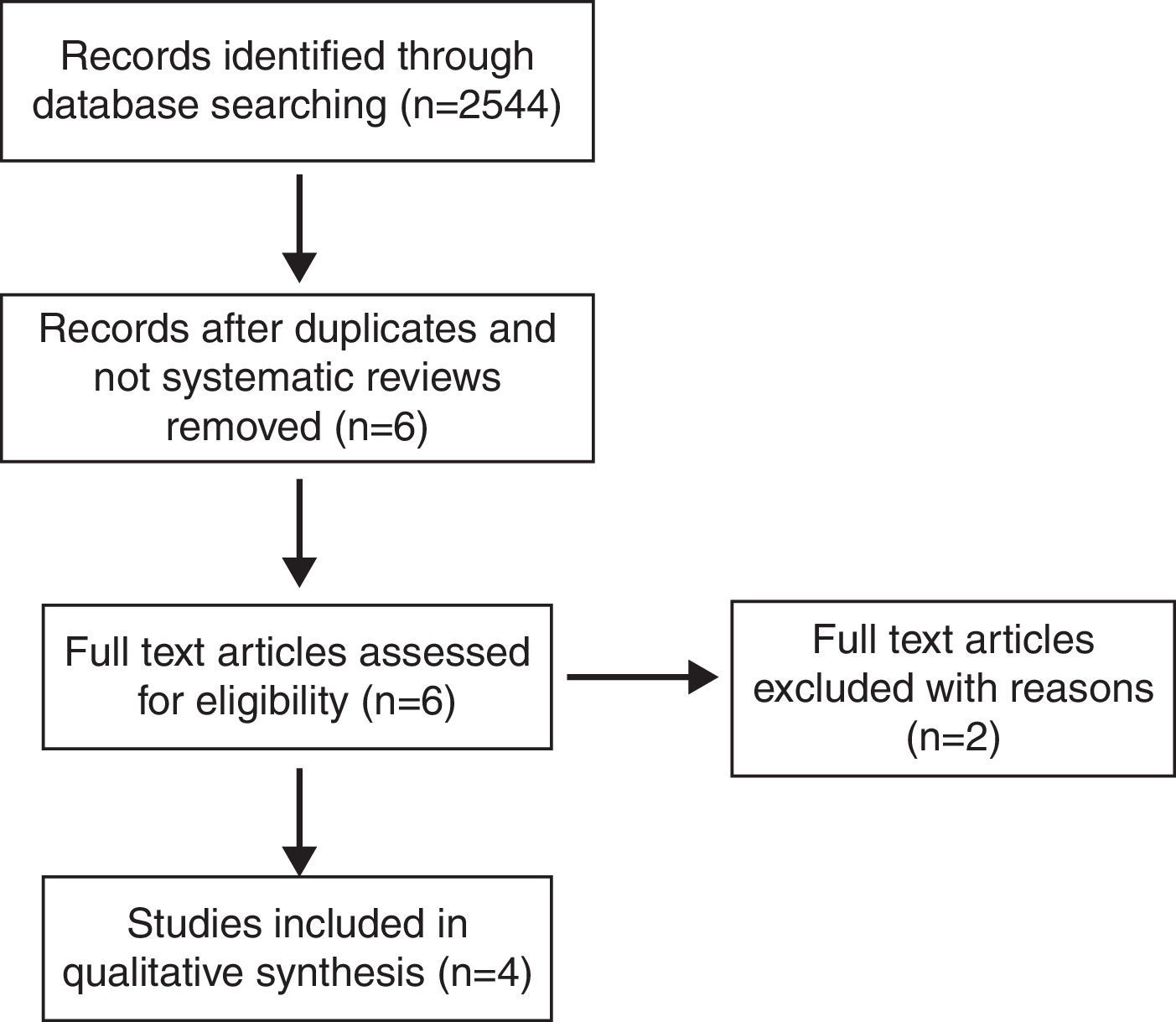
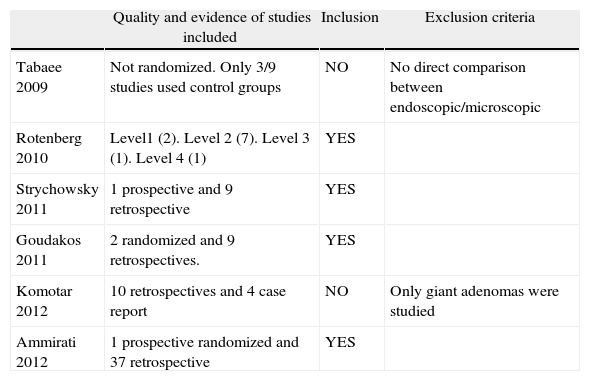
Materials and methodsWe carried out a bibliographic search on MEDLINE and EMBASE electronic databases, selecting those systematic reviews and meta-analyses published from the year 2000 until January 2013, focusing on comparisons between microsurgical and endoscopic techniques.
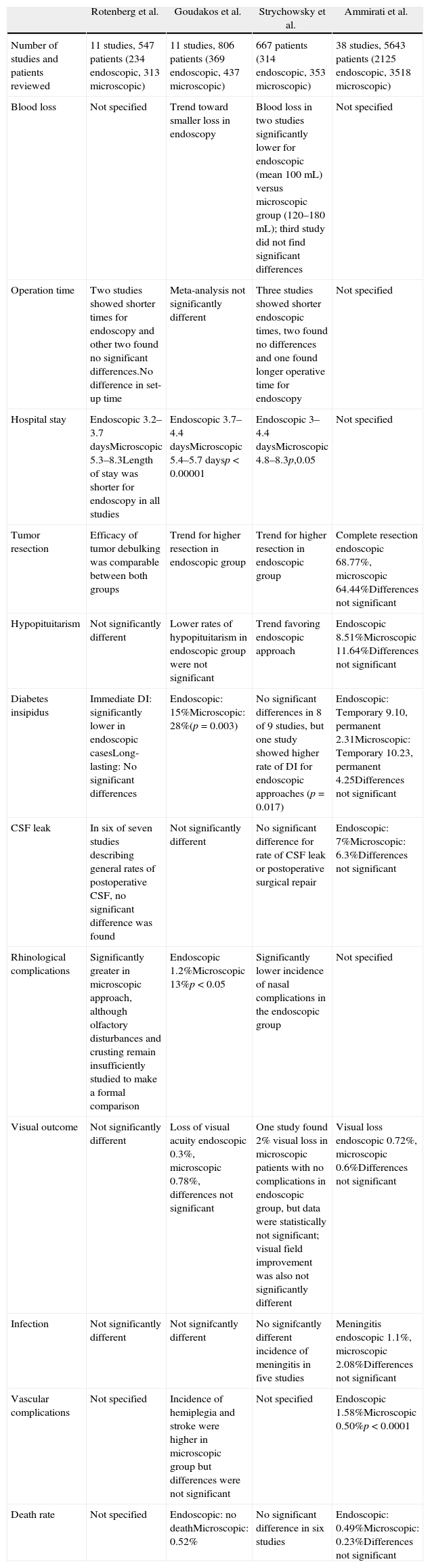
ResultsWe concluded with type A consistency that hospital stay was shorter and diabetes insipidus and rhinological complications were less frequent in the endoscopy group. We concluded with type B consistency that lower rates of patient blood loss, shorter operative times, higher rate of gross total resection, lesser association to visual impairment and lower rate of hypopituitarism were observed in the endoscopy group. Vascular complications and cerebrospinal fluid fistulas were reduced with microsurgery. It is crucial to perform a combined analysis of all the systematic reviews treating a specific topic, observing and analysing the trends and how these are affected by new contributions.
ConclusionRandomized multicenter studies are necessary to resolve the controversy over endoscopic and microsurgical approaches in hypophyseal pathology.
Las técnicas endoscópicas aplicadas a la cirugía hipofisaria han experimentado un importante desarrollo en los últimos años. Nuestro objetivo es realizar un examen de las diferentes revisiones sistemáticas publicadas en la literatura inglesa, para determinar la consistencia y las conclusiones alcanzadas tras la comparativa entre abordajes endoscópicos y microscópicos en la cirugía hipofisaria.
Material y métodosSe ha realizado una revisión de la literatura inglesa utilizando las bases de datos MEDLINE y EMBASE, seleccionando las revisiones sistemáticas y metaanálisis publicados desde el año 2000 al 2013, focalizándonos en la comparativa entre los abordajes endoscópicos y microscópicos para el tratamiento de patología hipofisaria.
ResultadosConcluimos con consistencia tipo A que la estancia hospitalaria fue más corta, así como la diabetes insípida y las complicaciones rinológicas fueron menos frecuentes en el grupo endoscópico. Encontramos consistencia tipo B a favor de que la pérdida hemática es menor, el tiempo quirúrgico es más corto, la tasa de resección completa es mayor, el deterioro visual es menos frecuente y la tasa de hipopituitarismo es menor en el grupo endoscópico. Las complicaciones vasculares y la fístula de LCR fueron menos frecuentes en el grupo microscópico con consistencia tipo B. Resulta fundamental realizar un análisis combinado de todas las revisiones sistemáticas que tratan un tema específico, observando y analizando las tendencias y cómo estas se pueden ver afectadas por las nuevas contribuciones.
ConclusionesEstudios aleatorizados multicéntricos son necesarios para resolver la controversia entre el tratamiento endoscópico y microscópico de la patología hipofisaria.
Article

If it is the first time you have accessed you can obtain your credentials by contacting Elsevier Spain in suscripciones@elsevier.com or by calling our Customer Service at902 88 87 40 if you are calling from Spain or at +34 932 418 800 (from 9 to 18h., GMT + 1) if you are calling outside of Spain.
If you already have your login data, please click here .
If you have forgotten your password you can you can recover it by clicking here and selecting the option ¿I have forgotten my password¿.