The 30-day readmission rate has become an important indicator of health care quality. This study focuses on the incidence of 30-day readmission in neurosurgical patients and related risk factors.
Material and methodsA retrospective review was performed on patients treated in a neurosurgery department between 1 January 2012 and the 31 December 2013. Patients requiring readmission within 30 days of discharge and the readmission diagnosis were identified, and the factors related to their readmission were analysed.
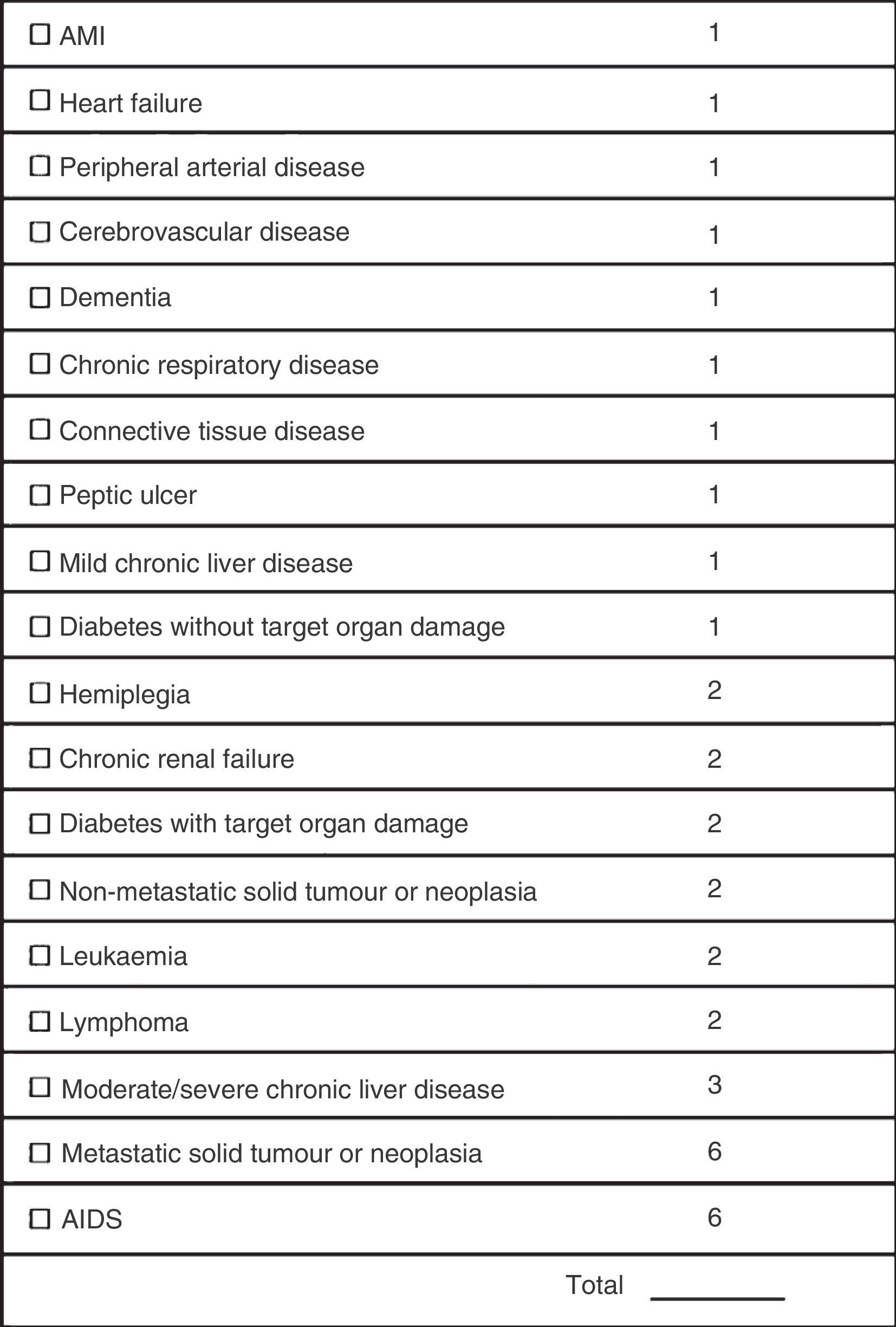
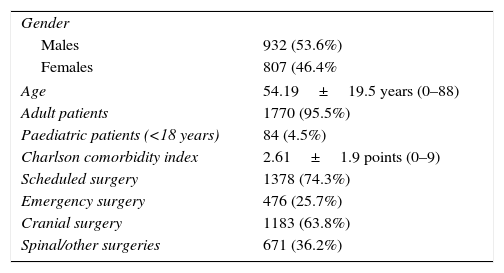
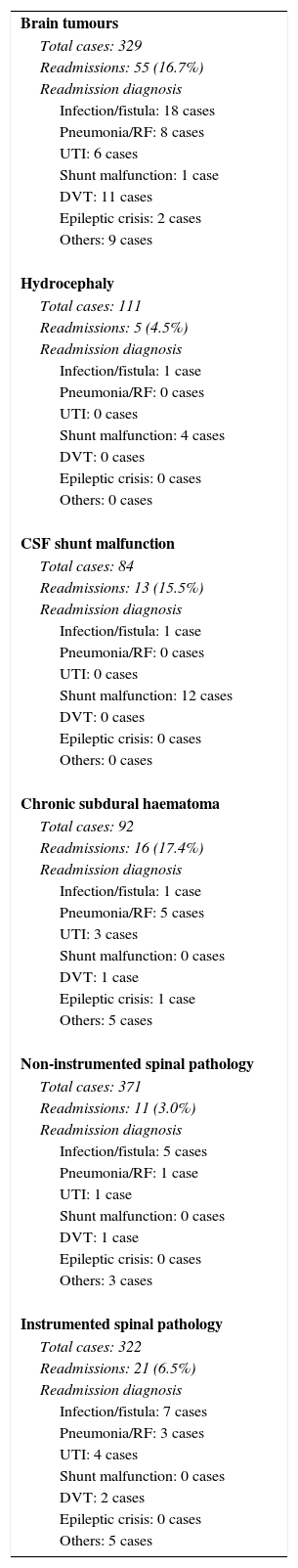
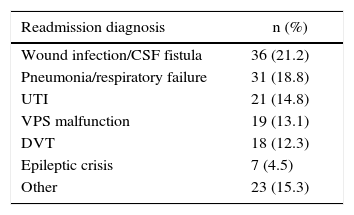
ResultsA total of 1854 interventions were carried out on 1739 patients during the aforementioned (study) period. Of the remaining patients, 174 (10.2%) required readmission within 30 days of discharge. The main causes of readmission were problems related to the surgical wound (21.2% of all readmissions), followed by respiratory processes (18.8%). A total of 73.9% of readmissions occurred in patients who had undergone cranial surgery. Multiple comorbidities estimated by Charlson comorbidity index and length of hospital stay were identified as factors related to a higher readmission rate.
ConclusionsThe 30-day readmission rate observed in our series was 10.2%. Multiple comorbidity expressed by the Charlson comorbidity index and length of hospital stay were related to readmission.
El reingreso a los 30días se ha convertido en un parámetro de uso creciente como indicador de calidad asistencial. El presente trabajo pretende establecer la frecuencia de reingreso a los 30días entre pacientes que precisaron intervención neuroquirúrgica, así como analizar los factores relacionados con dicha eventualidad.
Material y métodosSe han revisado de forma retrospectiva los pacientes intervenidos en nuestra institución desde el 1 de enero de 2012 hasta el 31 de diciembre de 2013. Se han identificado los pacientes que precisaron reingreso en los primeros 30días tras recibir el alta hospitalaria, así como la causa que motivó dicho ingreso. Se han analizado los factores relacionados con el reingreso.
ResultadosSe llevaron a cabo 1.854 intervenciones en 1.739 pacientes durante el período señalado. Durante el ingreso fallecieron 36 pacientes (2,1%). De los pacientes restantes, un total de 174 (10,2%) precisaron reingreso hospitalario en los primeros 30días tras el alta. La principal causa de reingreso estuvo representada por los problemas relacionados con la herida quirúrgica (21,2% del total de reingresos), seguida de los procesos respiratorios (18,8%). El 73,9% de los reingresos aconteció en pacientes en los que se había realizado cirugía craneal. Los factores relacionados con una mayor tasa de reingreso fueron la comorbilidad múltiple estimada por el índice de comorbilidad de Charlson y la duración de la estancia hospitalaria anterior al reingreso.
ConclusionesEn nuestra serie el 10,2% de los pacientes precisaron nuevo ingreso hospitalario a los 30días. La comorbilidad múltiple expresada por el índice de comorbilidad de Charlson y la duración de la estancia hospitalaria estuvieron relacionados con dicha eventualidad.
Article

If it is the first time you have accessed you can obtain your credentials by contacting Elsevier Spain in suscripciones@elsevier.com or by calling our Customer Service at902 88 87 40 if you are calling from Spain or at +34 932 418 800 (from 9 to 18h., GMT + 1) if you are calling outside of Spain.
If you already have your login data, please click here .
If you have forgotten your password you can you can recover it by clicking here and selecting the option ¿I have forgotten my password¿.