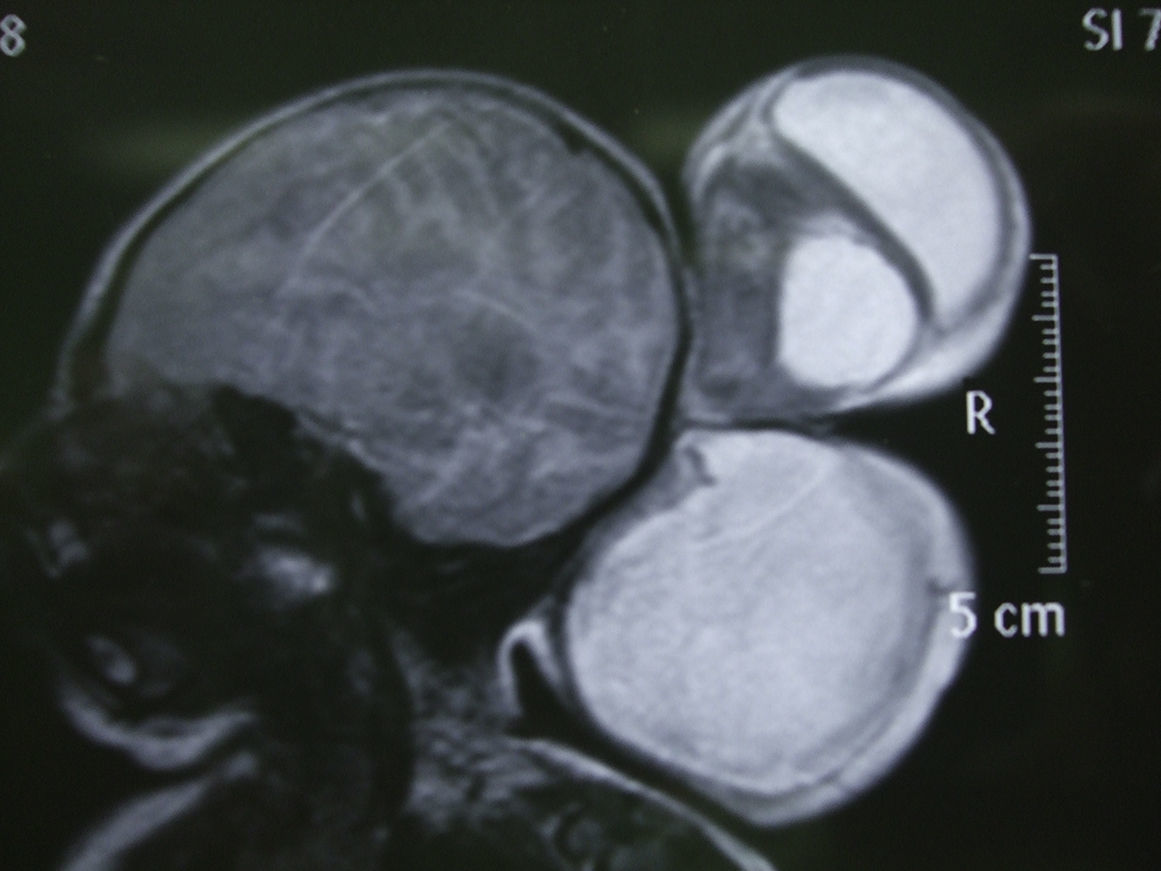
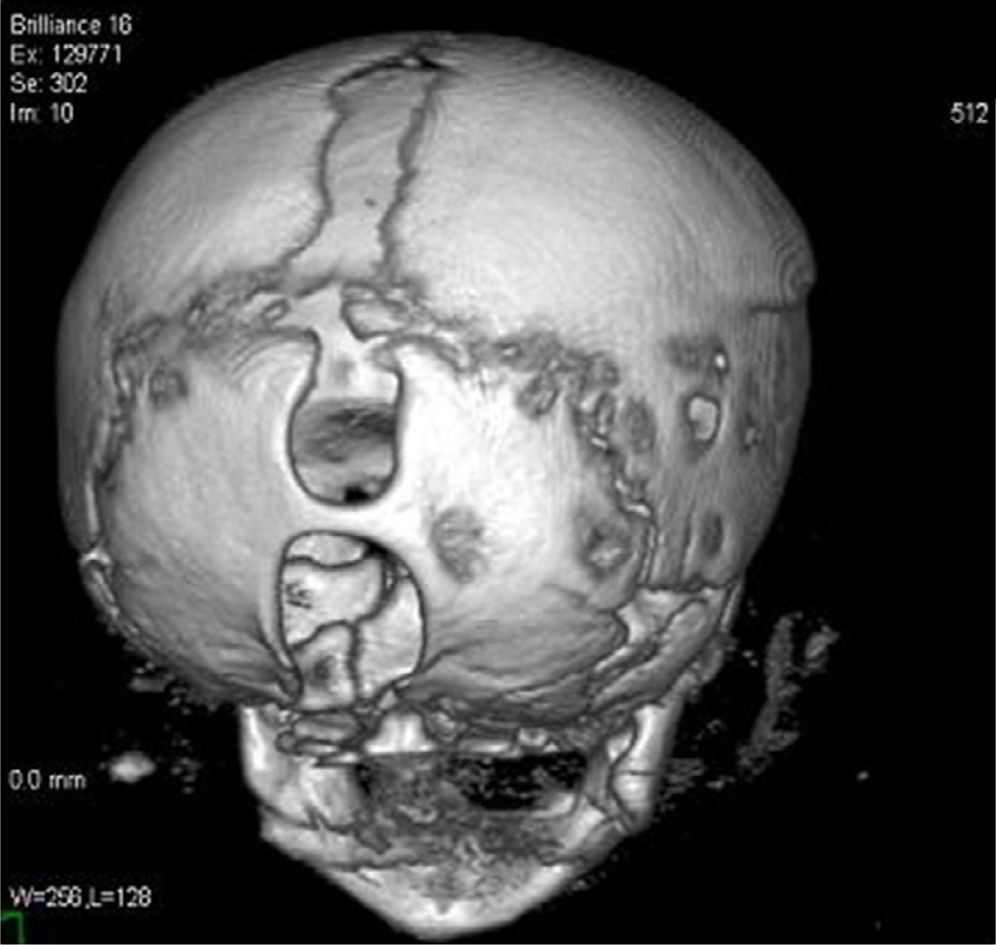
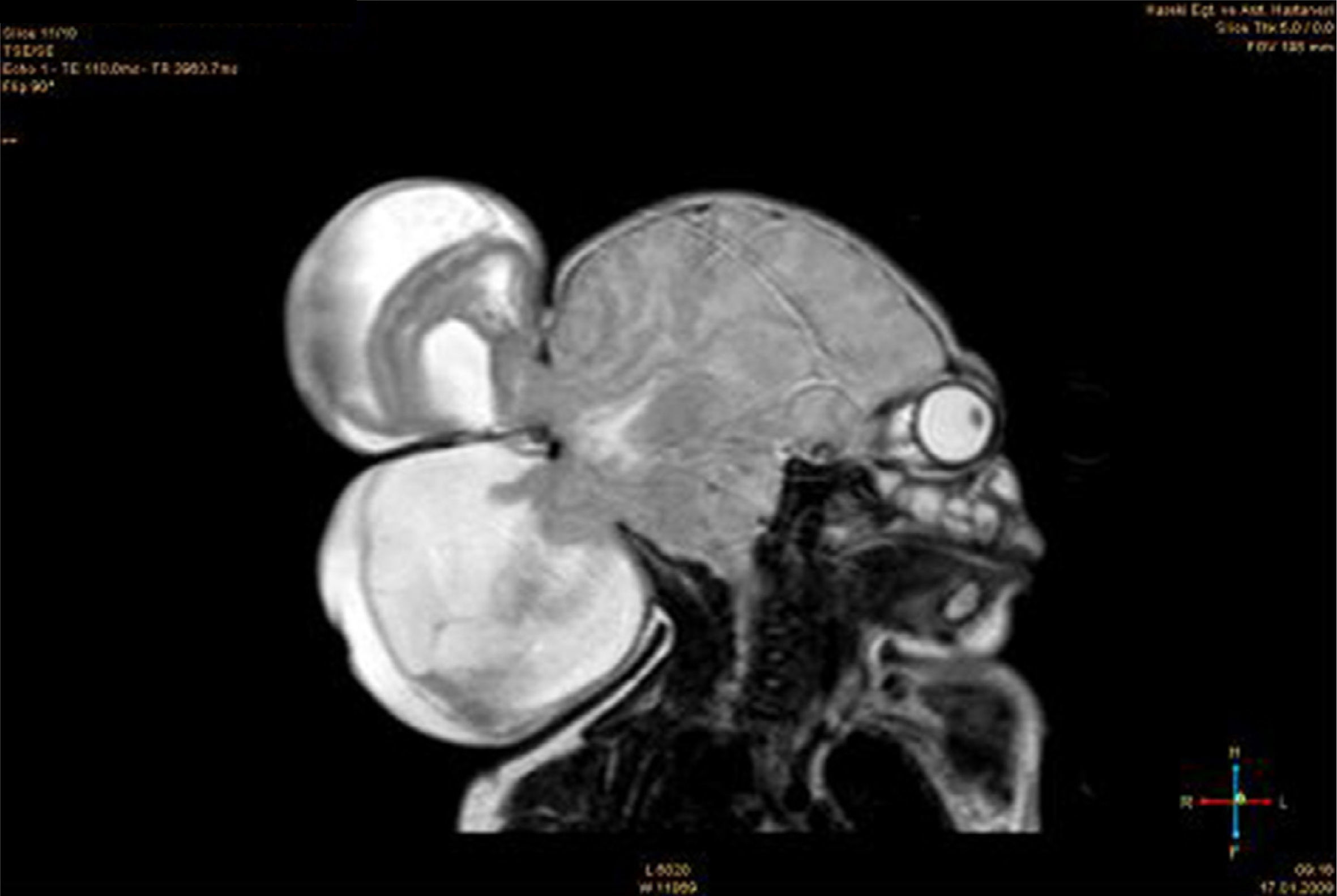
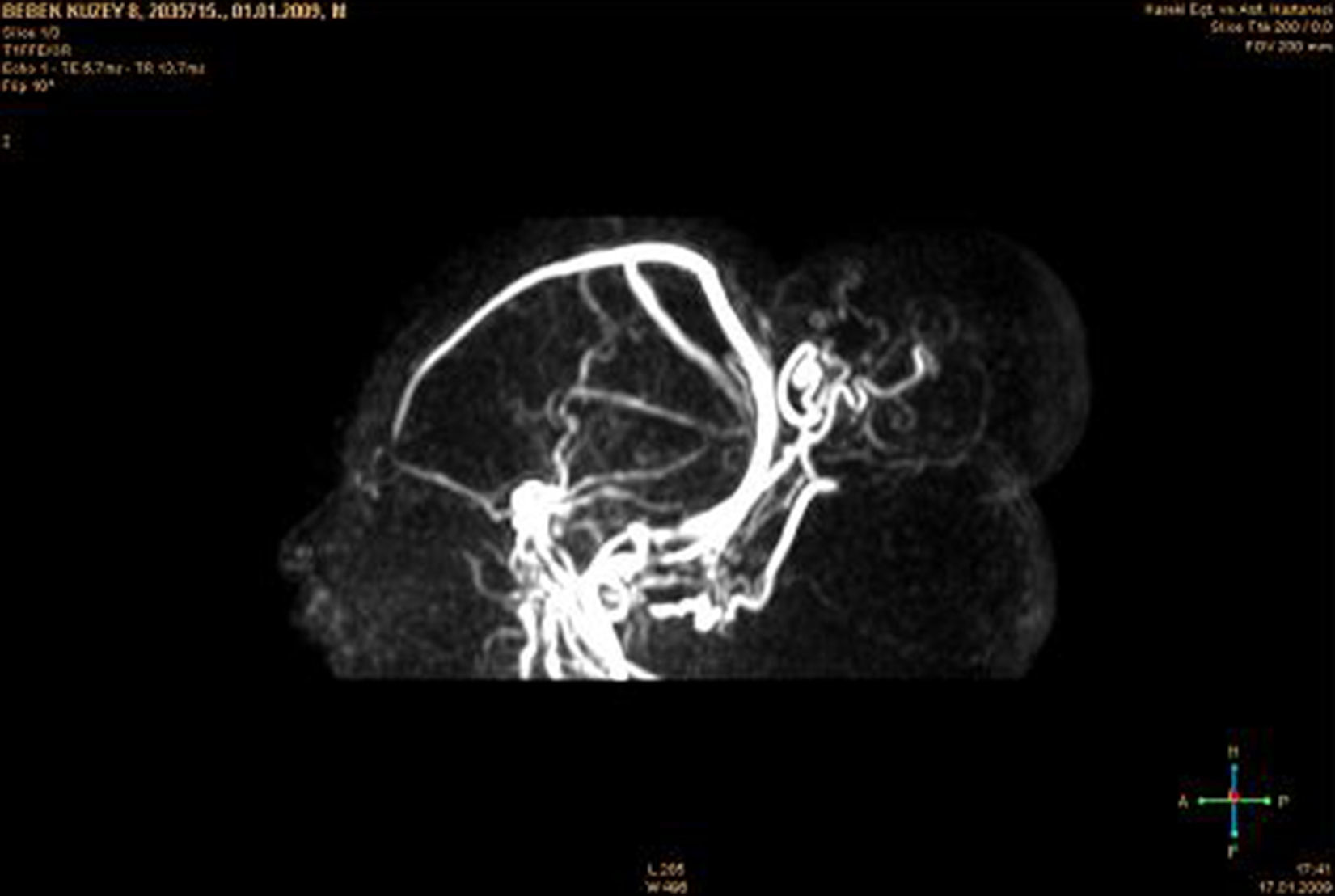
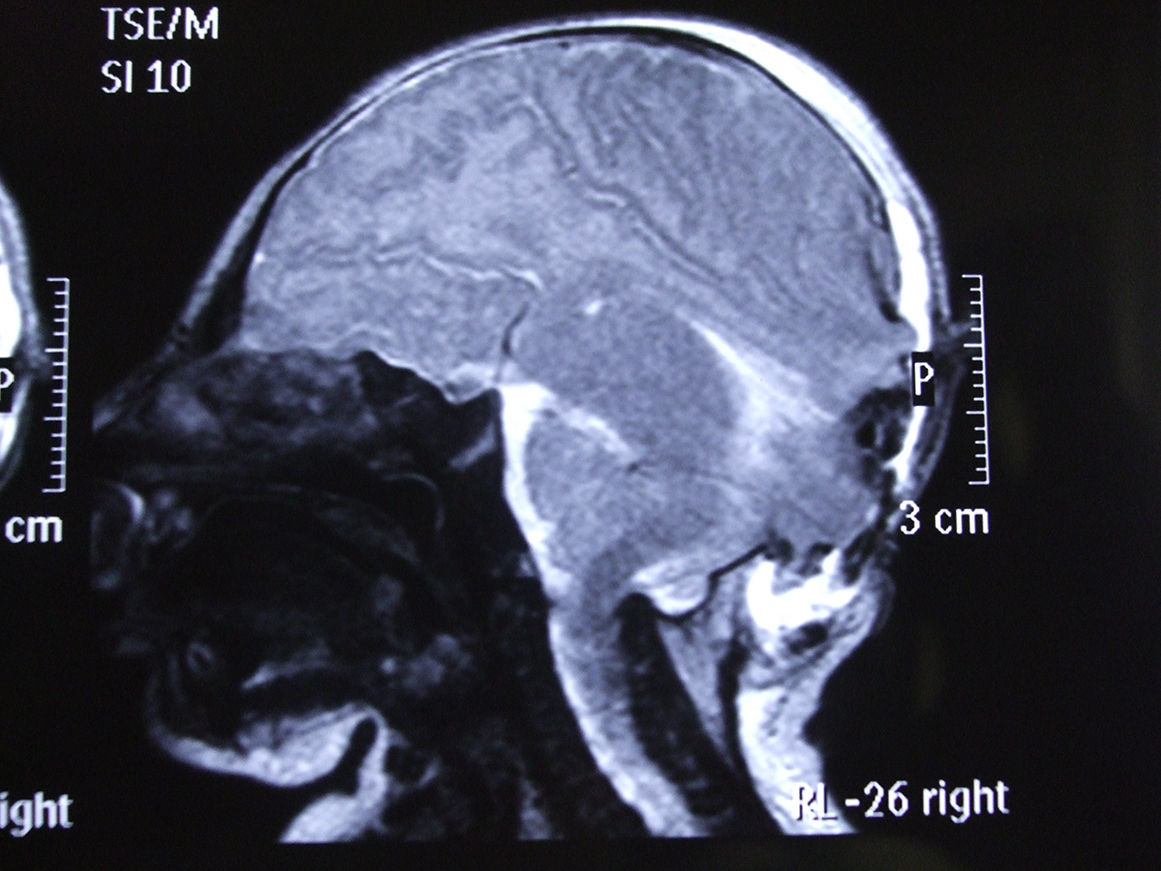
An encephalocele is a protrusion of the brain and/or meninges through a defect in the skull that is closed or covered with skin. Occipital encephaloceles are the most frequent type in North America and Western Europe, where about 85% of encephaloceles take this form. To the best of our knowledge, there are only three other reported cases of double occipital encephaloceles in the literature. The current study reports a double and both supra- and infra-torcular occipital encephalocele in a neonate and discusses the importance of preoperative neuroimaging studies to optimize the outcome. The patient was a 1-day-old male child who was identified by prenatal ultrasound to have two occipital encephaloceles. The patient underwent a closure of the occipital encephalocele on the second postnatal day. The infant tolerated the procedure well and was extubated on the first postoperative day. The child continues to do well during follow-up.
Un encefalocele es una protrusión del cerebro o de las meninges a través de un defecto craneal que está cerrado o cubierto con la piel. El encefalocele occipital es el tipo más frecuente en EE. UU. y Europa occidental, donde alrededor del 85% de los casos de encefalocele adoptan esta forma. Según nuestro conocimiento, solo existen publicados otros 3 casos de encefalocele occipital doble en la literatura. El presente estudio describe un encefalocele occipital doble en un neonato que además se presentaba tanto supra- como infratorcular. También se analiza la importancia de los estudios de neuroimagen preoperatorios para optimizar los resultados. El paciente, un varón de un día, presentaba 2 encefaloceles occipitales identificados mediante ecografía prenatal. Fue sometido a un cierre del encefalocele occipital en el segundo día posnatal. El niño toleró bien el procedimiento, fue extubado en el primer día del postoperatorio y sigue bien durante el seguimiento.
Article

If it is the first time you have accessed you can obtain your credentials by contacting Elsevier Spain in suscripciones@elsevier.com or by calling our Customer Service at902 88 87 40 if you are calling from Spain or at +34 932 418 800 (from 9 to 18h., GMT + 1) if you are calling outside of Spain.
If you already have your login data, please click here .
If you have forgotten your password you can you can recover it by clicking here and selecting the option ¿I have forgotten my password¿.