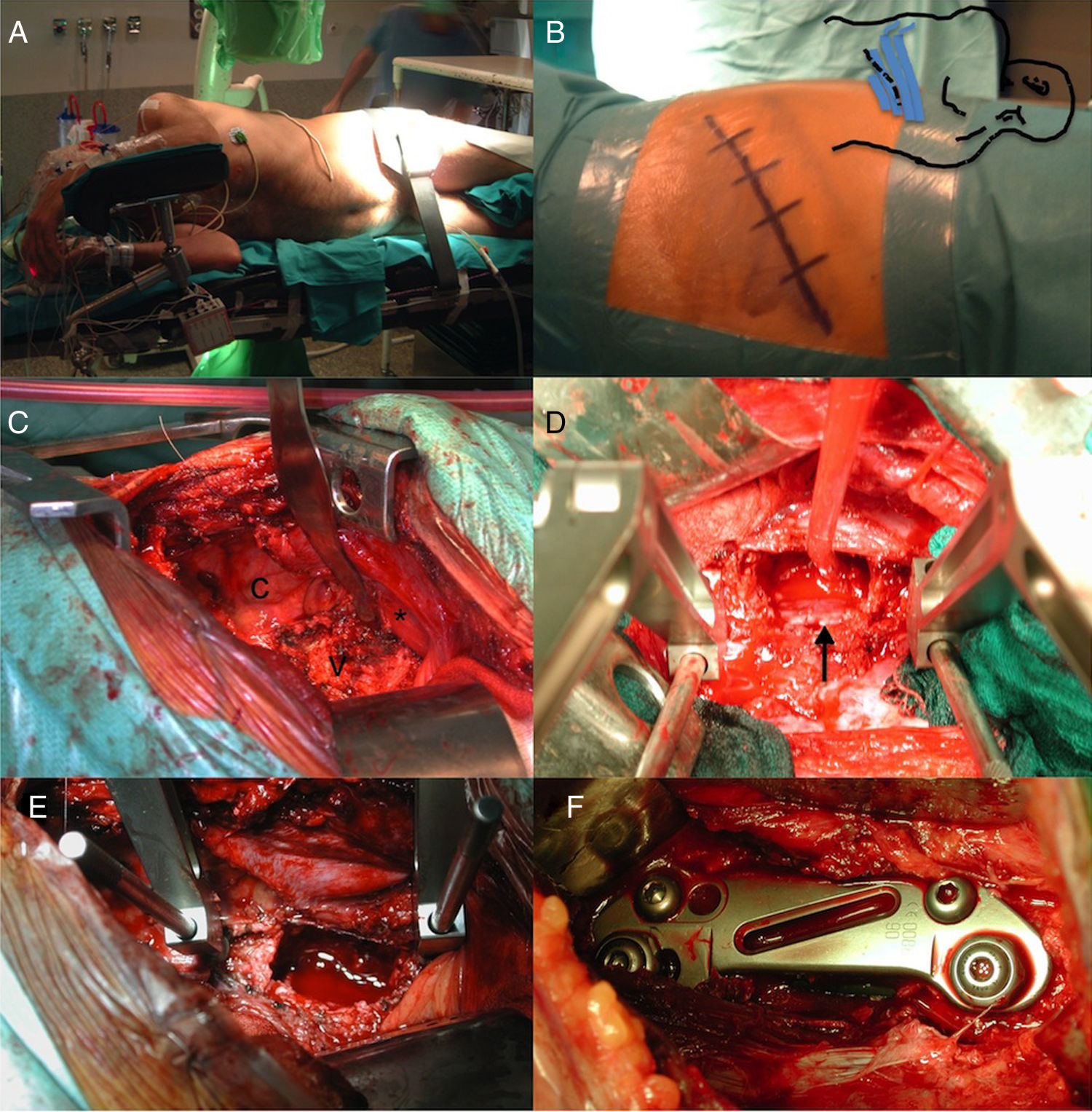
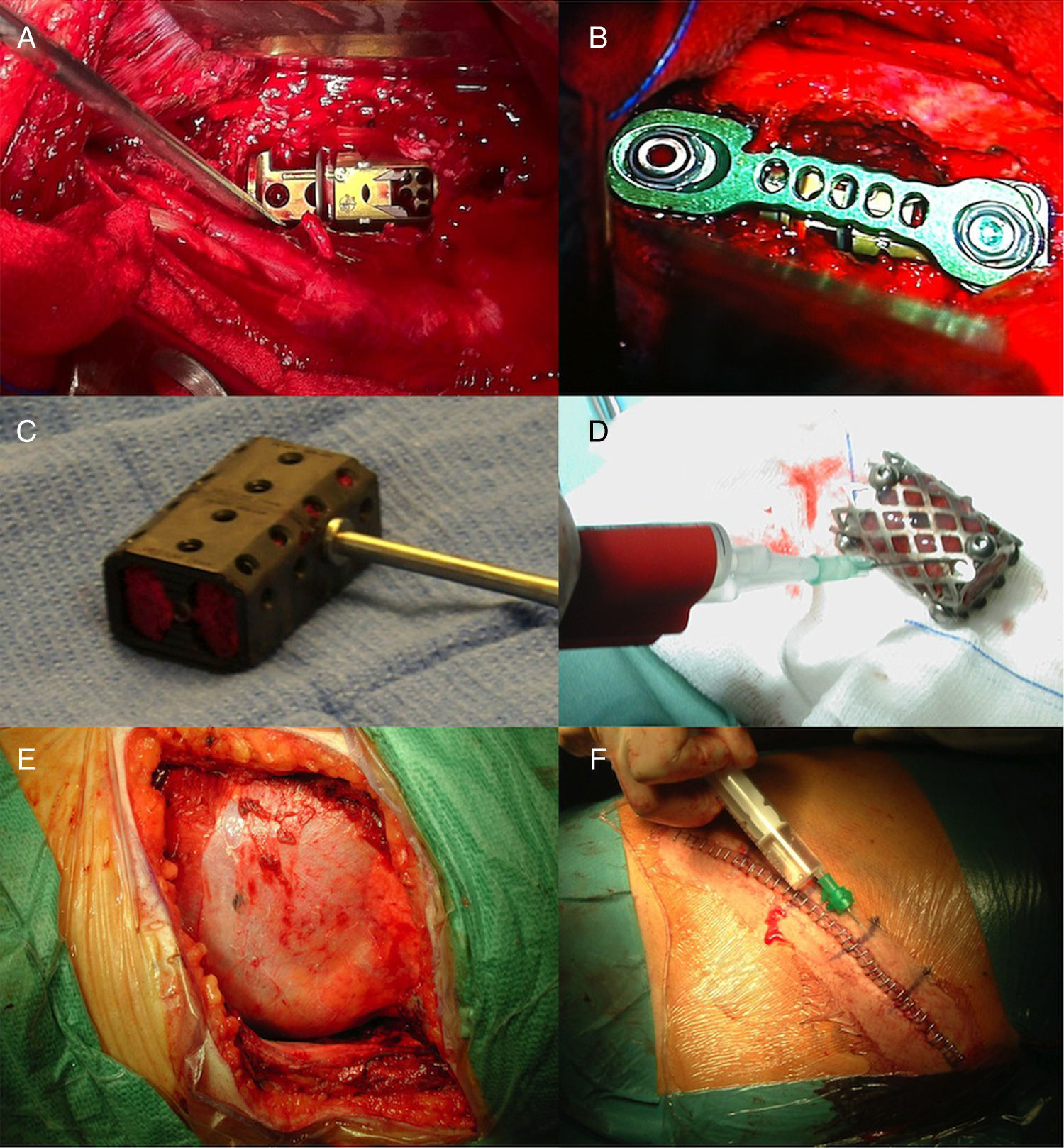
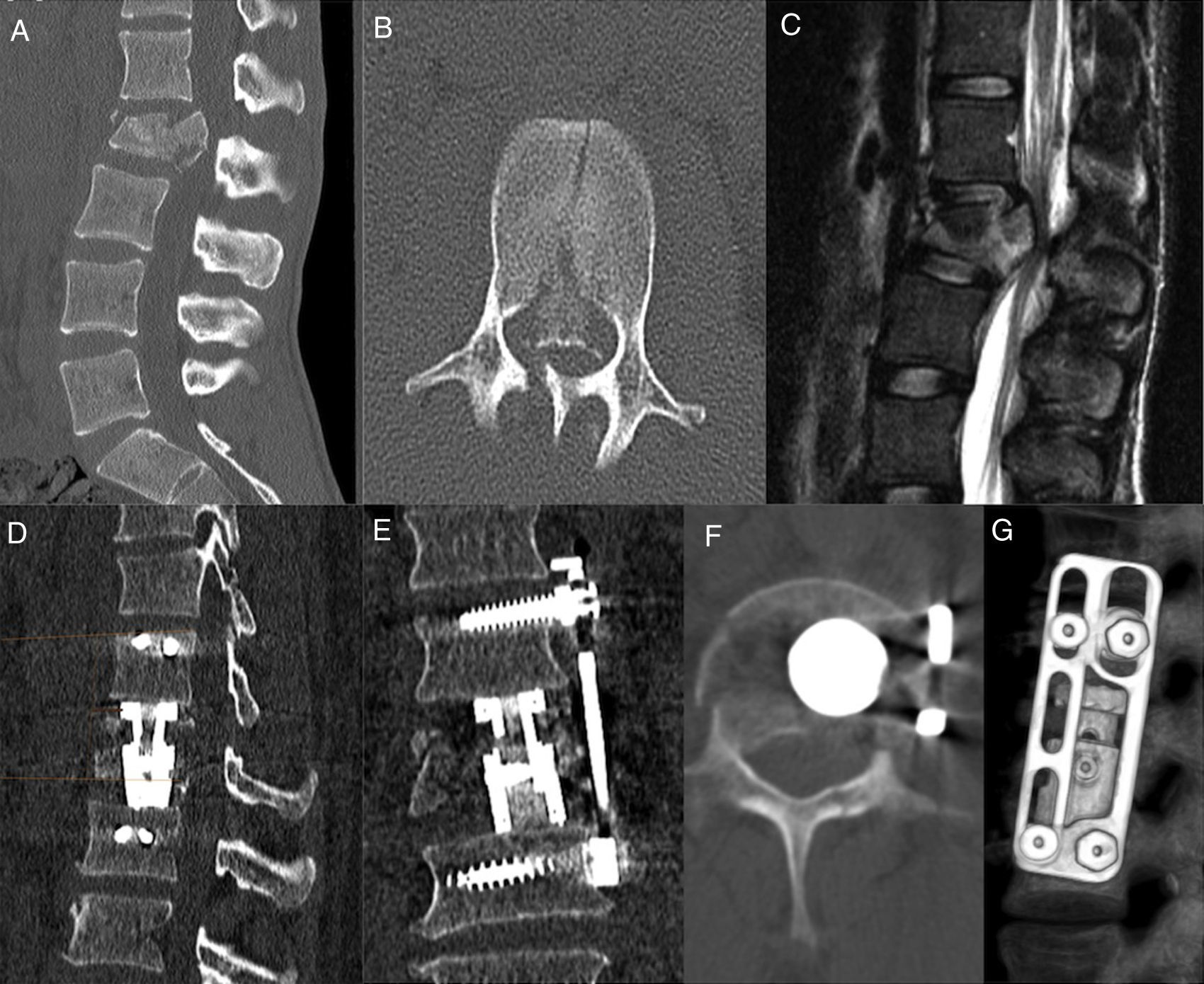
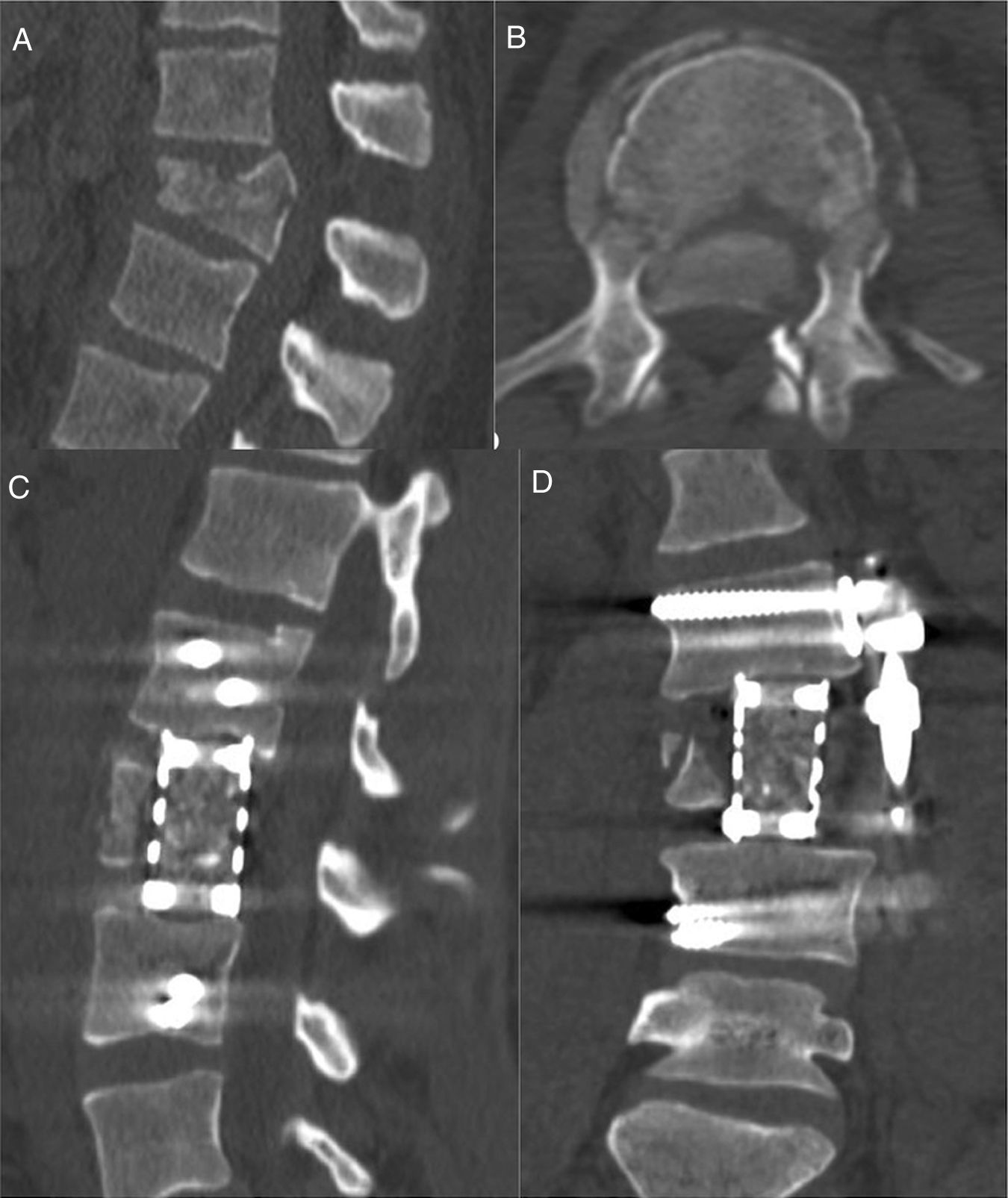
To describe the rationale, pros and cons, and complications of the anterior-lateral extrapleural retroperitoneal approach for unstable (TLICS>4) thoracolumbar fractures.
Patients and methodsClinical and radiological data and outcomes from a cohort treated surgically via said approach were retrospectively reviewed. All patients were operated on exclusively by 5 neurosurgeons trained in spine surgery.
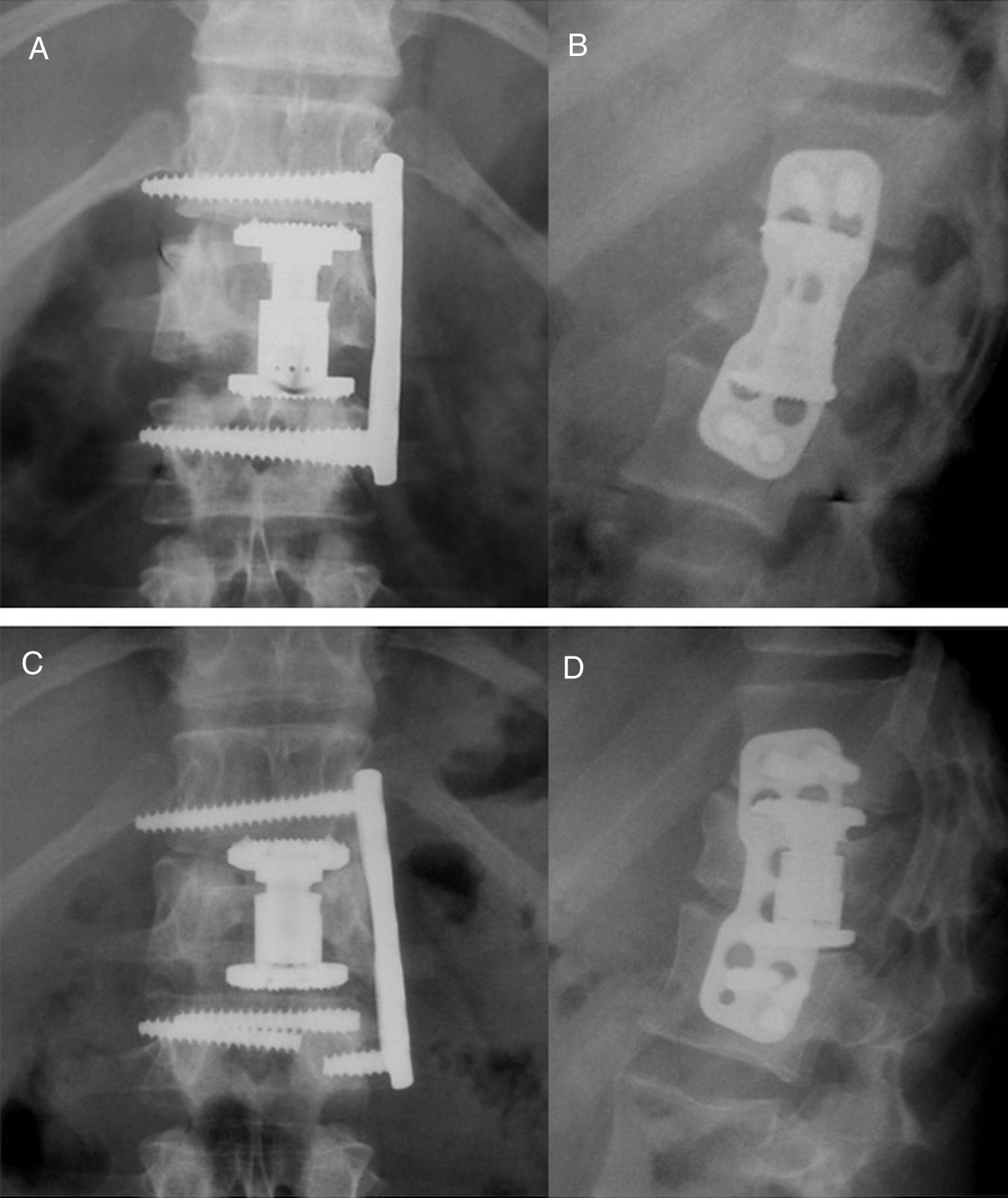
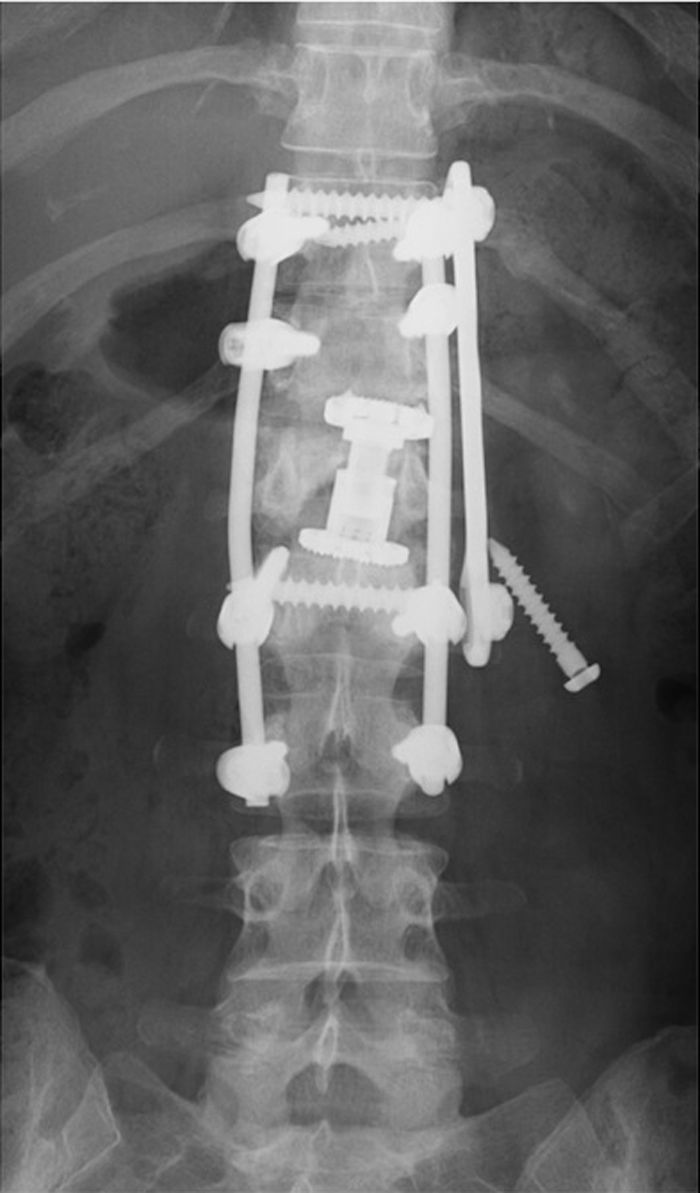
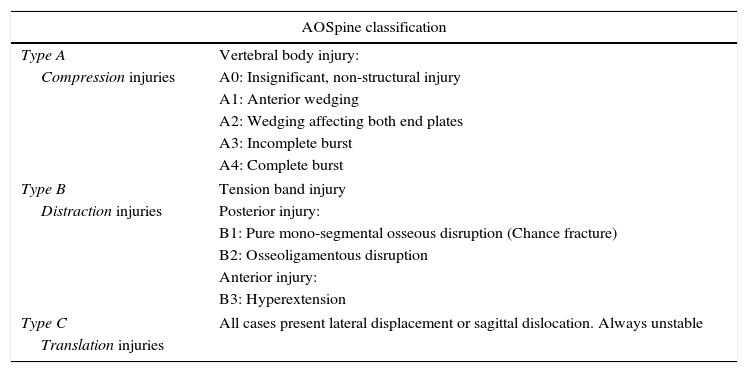
ResultsBetween June 1999 and December 2015, 86 patients underwent surgery (median age 42 years, most common level: L1). Approximately 32.5% presented with a preoperative neurological defect. After surgery (mean duration: 275min), 75.6% presented with no neurological sequelae and only one-third required blood transfusion. Median postoperative stay was 7 days. Correction of kyphosis was considered adequate and suboptimal but acceptable in 91% and 9% of the patients, respectively. Complications occurred in 36 patients, the majority being transient. We observed failure of the construct in 2 cases (collapse of an expandable cage and extrusion of a locking screw). No infections, vascular or visceral lesions, permanent neurological worsening or mortality occurred during hospitalisation. One patient ultimately needed additional posterior fixation due to persistence of pain. Median follow-up was 252days (27.9% was lost to follow-up).
ConclusionsThe extrapleural extraperitoneal approach provides solid anterior reconstruction, allows wide decompression of the spinal canal, and permits adequate and long-lasting correction of kyphosis. The rates of infection, construct failure, need for reoperation and vascular or visceral lesions are minimal.
Describir los fundamentos, las ventajas, los inconvenientes y las complicaciones del abordaje anterolateral extrapleural-extraperitoneal en fracturas toracolumbares inestables (TLICSS>4).
Pacientes y métodosSe evalúan retrospectivamente datos clínicos y radiológicos, resultados y complicaciones de una cohorte intervenida mediante dicho abordaje. Todos los pacientes fueron intervenidos exclusivamente por 5 neurocirujanos entrenados en cirugía de columna.
ResultadosUn total de 86 pacientes fueron intervenidos entre junio de 1999 y diciembre de 2015 (mediana de edad 42años y nivel más frecuente L1). El 32,5% presentaban defecto neurológico preoperatorio. Tras la intervención (duración media: 275min), el 75,6% quedaron sin secuelas neurológicas y solo un tercio de pacientes precisó transfusión. La estancia media postoperatoria fue de 7días. La corrección de la cifosis se consideró correcta y subóptima pero aceptable en el 91 y el 9% de los casos, respectivamente. Ocurrieron complicaciones en 36 pacientes, la gran mayoría transitorias. Se constataron 2 fallos de material (colapso de caja expansible y extrusión de tornillo de bloqueo). No ocurrieron infecciones, lesiones vasculares, lesiones viscerales, empeoramiento neurológico permanente ni mortalidad durante el ingreso. Un paciente precisó estabilización posterior tardía por persistencia del dolor. El seguimiento mediano fue de 252días (27,9% pérdidas).
ConclusionesEl abordaje extrapleural-extraperitoneal proporciona una estabilización anterior sólida, permite una amplia descompresión del canal y una corrección adecuada y duradera de la cifosis. Las tasas de infección, fallo del material, necesidad de reoperación y lesiones vasculares o viscerales son mínimas.
Article

If it is the first time you have accessed you can obtain your credentials by contacting Elsevier Spain in suscripciones@elsevier.com or by calling our Customer Service at902 88 87 40 if you are calling from Spain or at +34 932 418 800 (from 9 to 18h., GMT + 1) if you are calling outside of Spain.
If you already have your login data, please click here .
If you have forgotten your password you can you can recover it by clicking here and selecting the option ¿I have forgotten my password¿.