The anaplastic ganglioglioma (AG) is the high-grade counterpart of ganglioglioma, a rare mixed tumor composed of neuronal/ganglion and glial cells.
Materials and methodsWe describe the histopathology and immunohistochemistry in 7 cases of AG and correlate them with the clinical and radiological features.
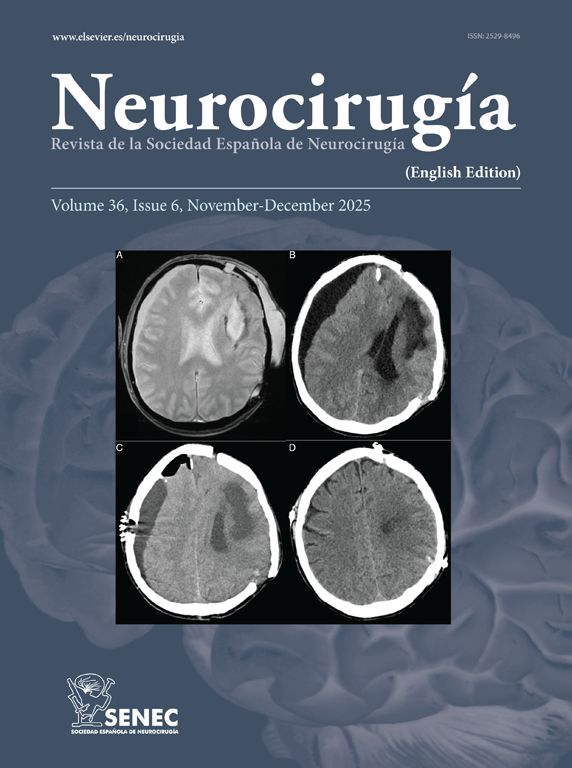
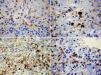
ResultsOur AG patients correspond to 2.5% of the central nervous system tumor patients evaluated in our institution. The mean age at presentation was 25.7 years, with a male predominance. The most common clinical presentation was generalized tonic–clonic seizures (3/7 cases), in correlation with frequent cortical/subcortical location (6/7 cases). Histopathologically, all our cases showed high-grade features in glial (glial fibrillary acid protein-positive) and neuron-ganglion cells (synaptophysin, PGP-9.5, neurofilament, NSE and CD56-positive), as well as moderate cellularity, frequent mitotic figures and a Ki-67 labeling index >5%. All our patients had poor survival.
ConclusionWe found that a typical histopathological and immunohistochemical profile is constant and can be useful in early diagnosis of these aggressive neoplasms.
El ganglioglioma anaplásico (GA) es la contraparte de alto grado del ganglioglioma, un raro tumor compuesto por una mezcla de células neuronales/ganglionares y gliales.
Materiales y métodosSe describe la histopatología y la inmunohistoquímica en 7casos de GA.
ResultadosLos casos de GA correspondieron al 2,5% de los tumores del SNC evaluados en nuestra institución. La edad media de presentación fue 25,7 años, con predominio del género masculino. La presentación más frecuente fue como convulsiones generalizadas tónico-clónicas (3/7casos), en correlación con una frecuente localización cortical/subcortical (6/7casos). Histopatológicamente todos los casos mostraron características de alto grado en las células gliales (GFAPpositivas) y ganglio/neuronales (sinaptofisina, PG-9.5, neurofilamentos, NSE y CD56-positivo), además de celularidad moderada, figuras mitóticas frecuentes y Ki-67>5%. Todos los pacientes mostraron baja supervivencia.
ConclusiónSe describe el perfil histopatológico e inmunohistoquímico en GA, el cual es constante y posee utilidad para el diagnóstico precoz de estos tumores agresivos.
Article

If it is the first time you have accessed you can obtain your credentials by contacting Elsevier Spain in suscripciones@elsevier.com or by calling our Customer Service at902 88 87 40 if you are calling from Spain or at +34 932 418 800 (from 9 to 18h., GMT + 1) if you are calling outside of Spain.
If you already have your login data, please click here .
If you have forgotten your password you can you can recover it by clicking here and selecting the option ¿I have forgotten my password¿.