Contralateral clipping of middle cerebral artery (MCA) aneurysms is not practiced widely and has been reported only in case series. Some of the neurosurgeons proposing this approach have even postulated that a short M1 segment is a basic requirement for performing it.
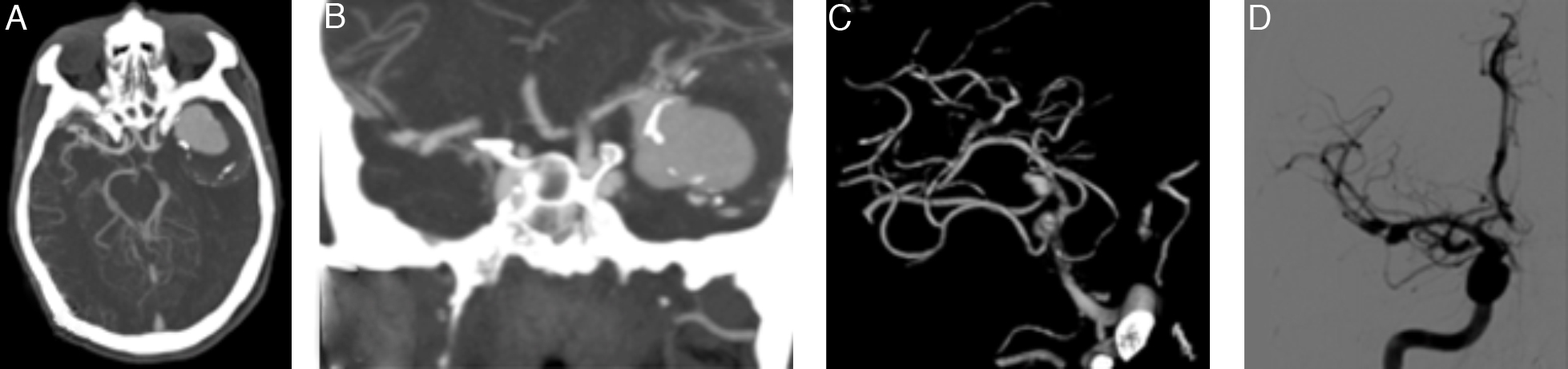
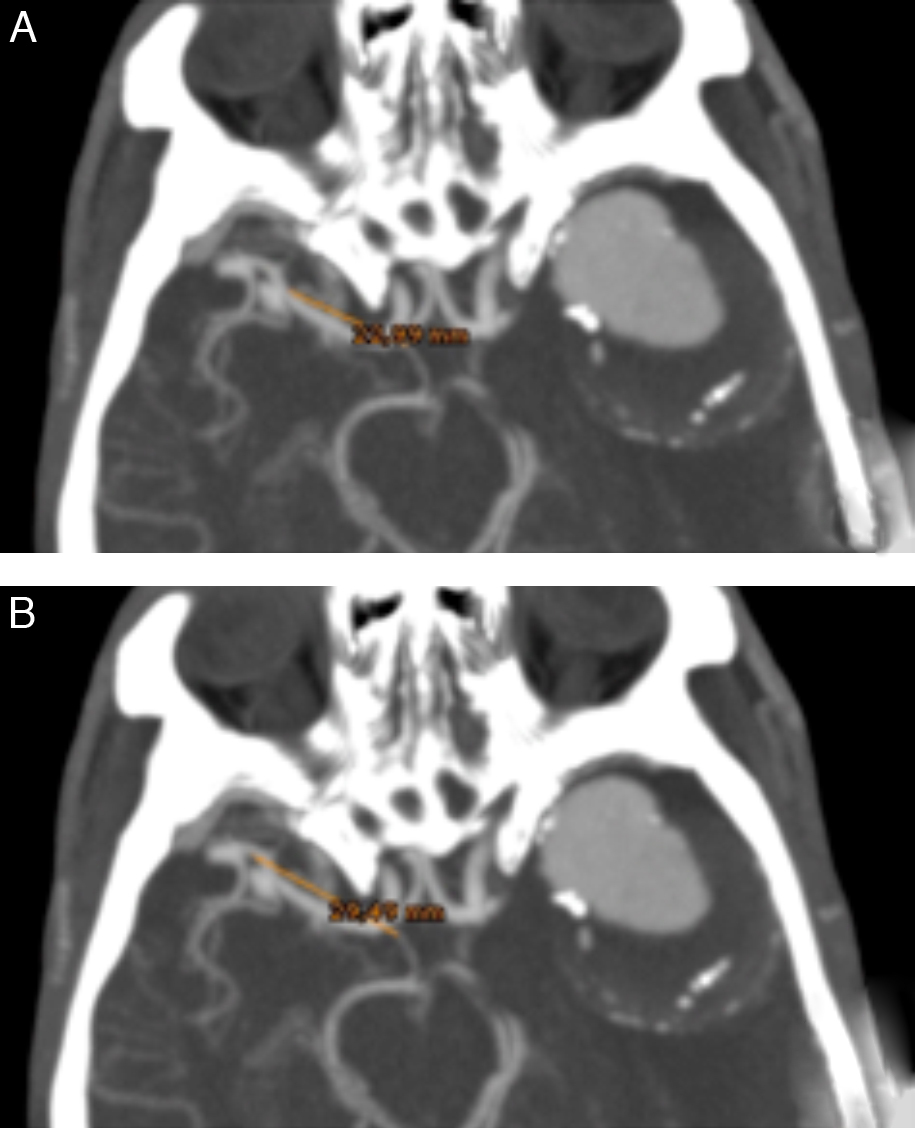
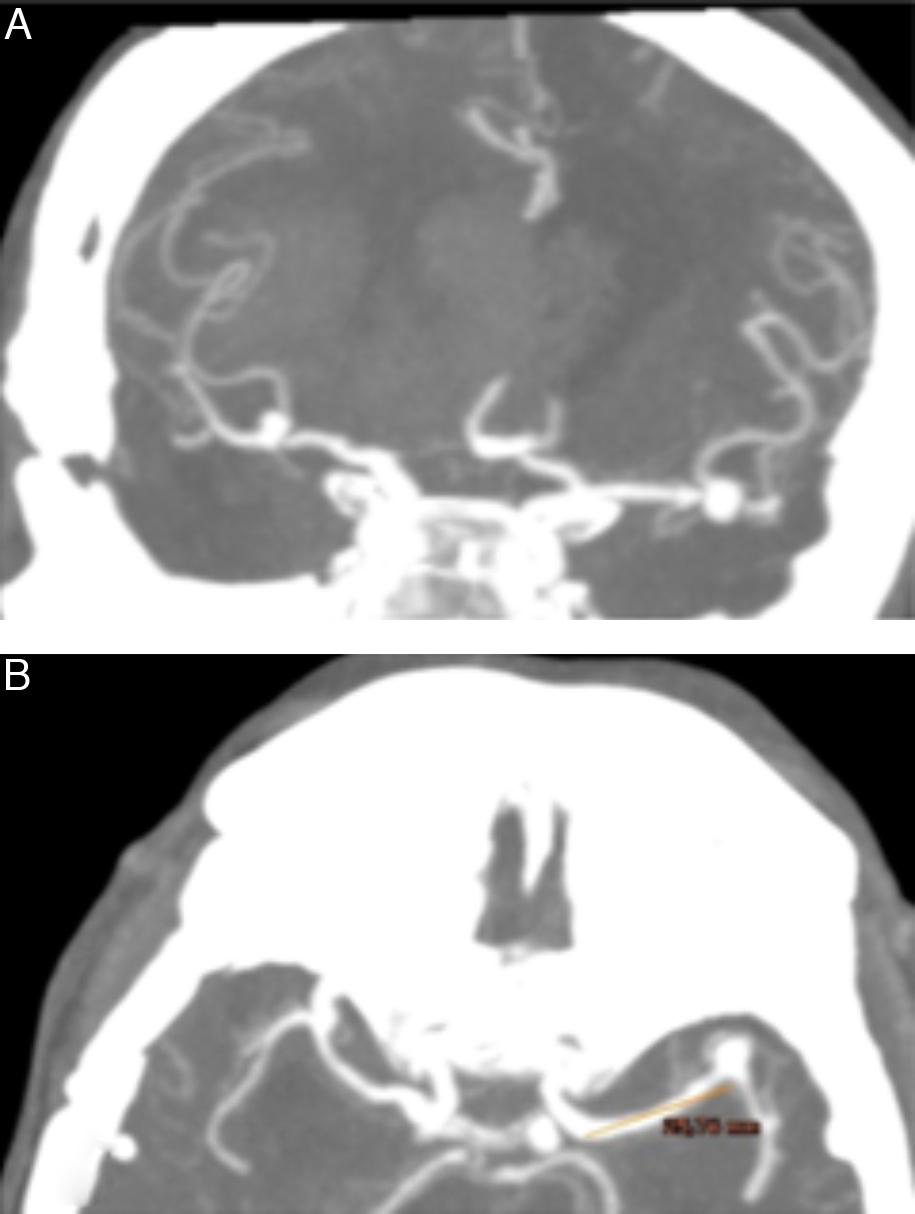
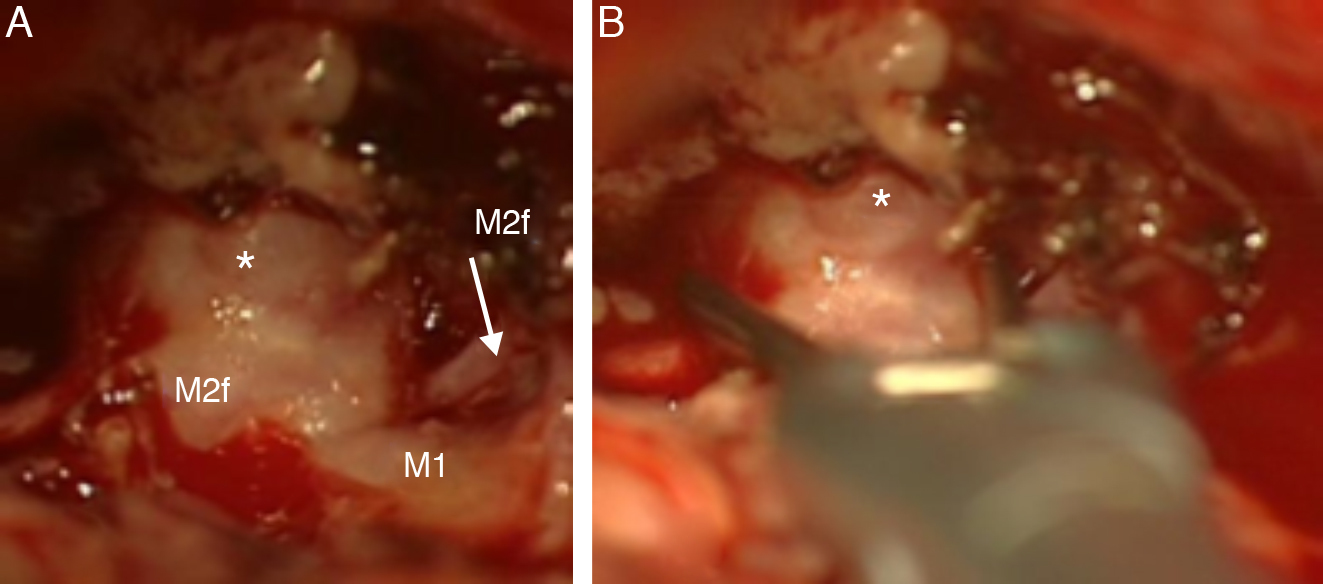
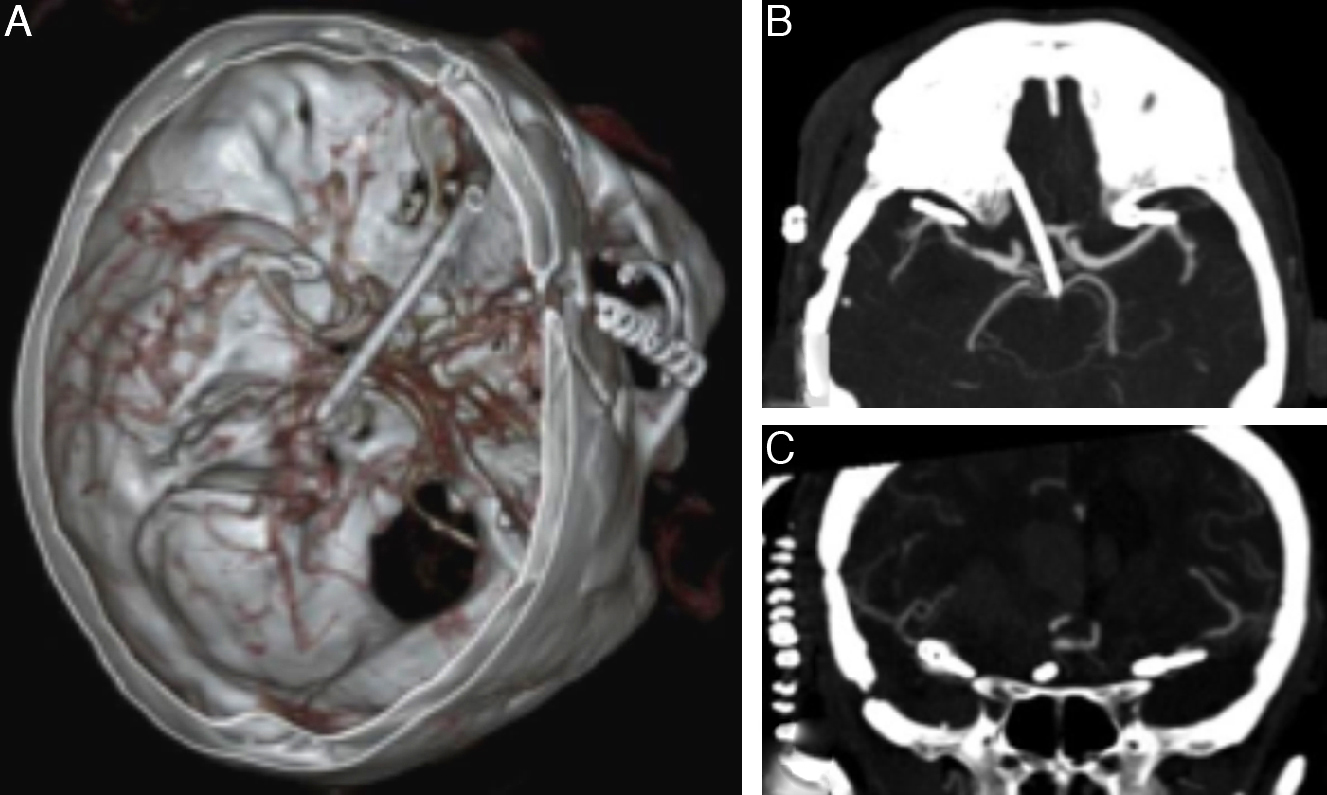
CasesWe present our experience using a contralateral approach with 2 patients who had 3 MCA aneurysms located more than 2.5cm from the carotid bifurcation. All 3 aneurysms were completely occluded, as demonstrated on postoperative CT angiography, and the patients’ neurological evolution was uneventful.
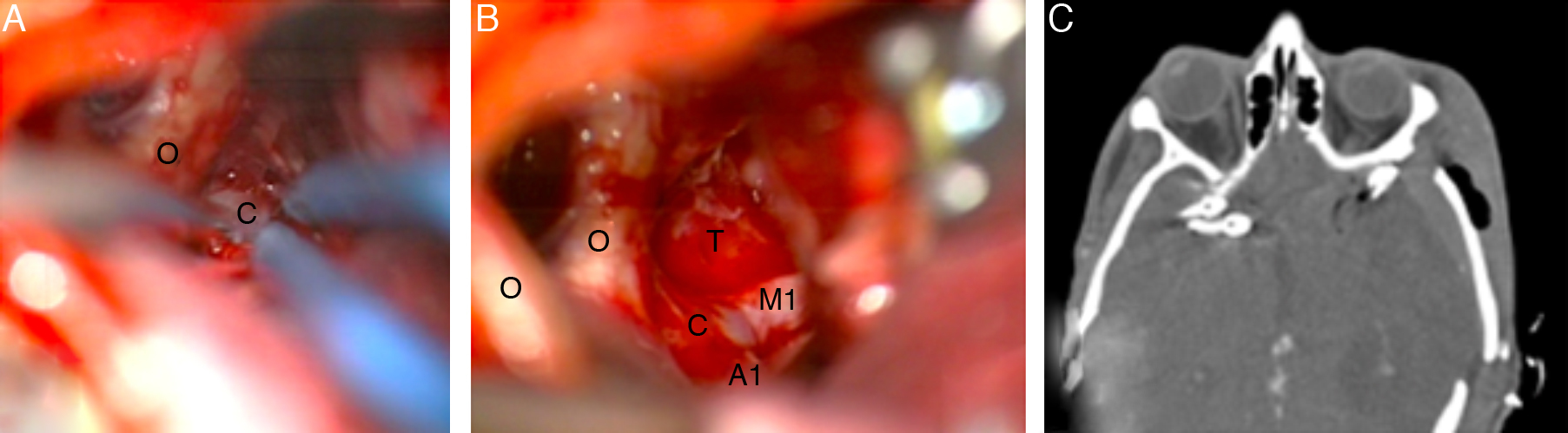
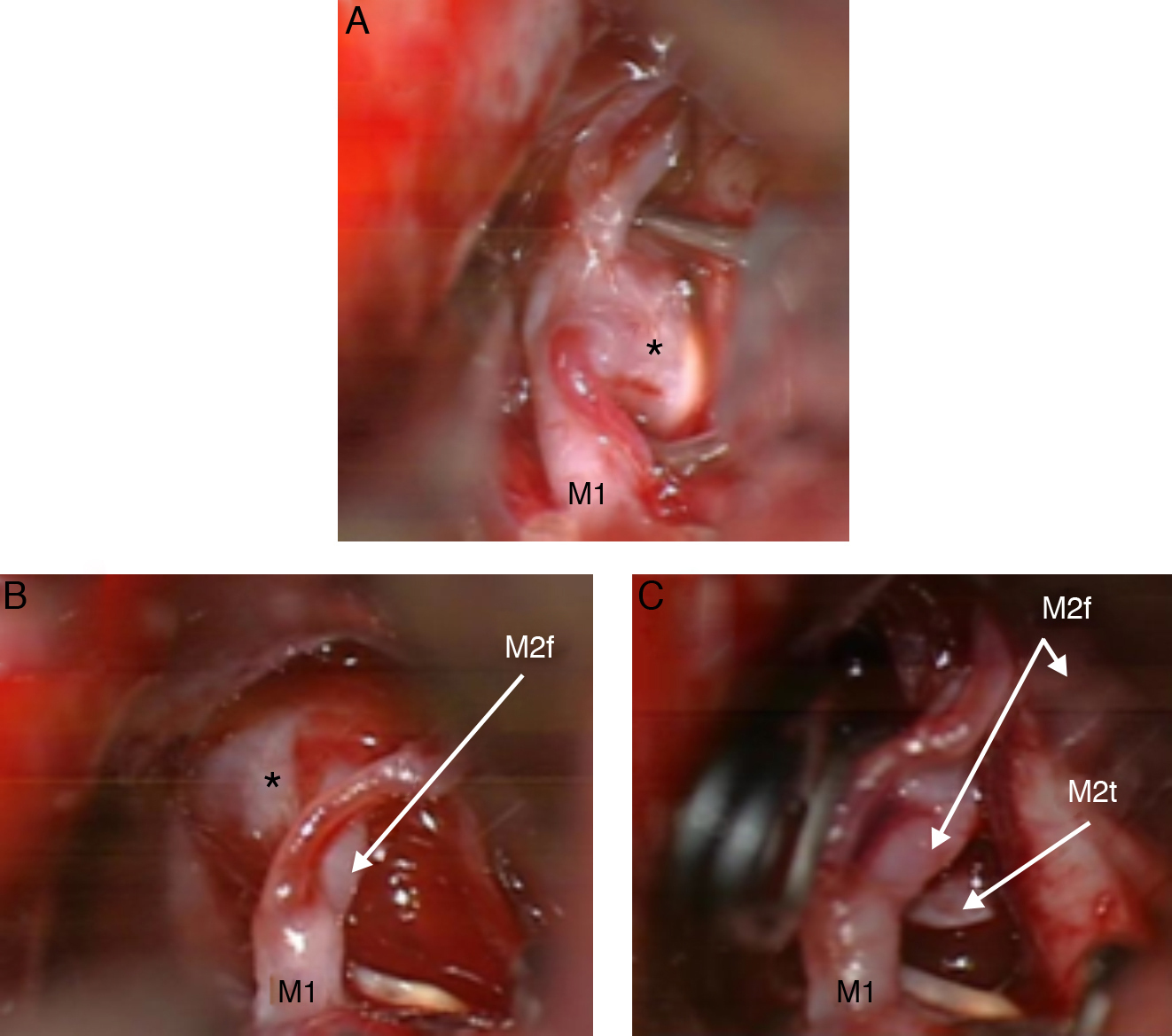
DiscussionThe contralateral approach can be regarded as a safe and effective technique for MCA aneurysm clipping. One contraindication frequently stated is the length of the MCA M1 segment; however, our experience proves that long distances can be reached if an adequate Sylvian fissure dissection is performed. We consider that the use of a contralateral approach requires fine technical skills and should be the choice only under judicious case-to-case planning, always bearing the preferences and experience of the neurosurgeon in mind.
El abordaje contralateral en aneurismas de la arteria cerebral media (ACM) no es muy utilizado, debido a las dificultades técnicas que plantea la distancia de disección tan larga. Incluso se ha promulgado que, en los casos en los que el segmento M1 de la ACM sea muy largo, estaría contraindicado el uso de este abordaje contralateral.
CasosPresentamos nuestra experiencia con tres aneurismas en dos pacientes a los que se realizó abordaje contralateral, pese a estar situados a más de 2,5cm de la bifurcación carotídea. En los tres aneurismas se comprobó el correcto pinzamiento mediante angio-tomografía computarizada postoperatoria y la evolución neurológica de los dos pacientes cursó sin complicaciones.
DiscusiónEl abordaje contralateral en aneurismas de la ACM es una técnica segura y eficaz. Con una buena disección de la cisura de Silvio, se pueden alcanzar distancias muy superiores a las propuestas en la bibliografía. Aun así, dada la mayor dificultad técnica de este abordaje contralateral, cada neurocirujano debe evaluar su utilización caso por caso, y siempre basándose en su experiencia y preferencias personales.
Article

If it is the first time you have accessed you can obtain your credentials by contacting Elsevier Spain in suscripciones@elsevier.com or by calling our Customer Service at902 88 87 40 if you are calling from Spain or at +34 932 418 800 (from 9 to 18h., GMT + 1) if you are calling outside of Spain.
If you already have your login data, please click here .
If you have forgotten your password you can you can recover it by clicking here and selecting the option ¿I have forgotten my password¿.